| Diabetic Retinopathy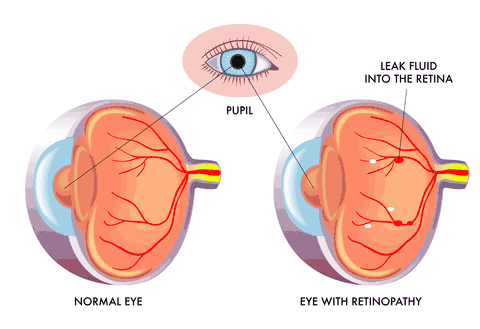 This corresponds to changes that become evident in the retina of a person that has diabetes mellitus. These changes start as small micro-aneurysms and can proceed to dot/blot hemorrhages, capillary closure, cotton wool spots, intra-retinal micro-vascular abnormalities, venous beading, lipid deposits, retinal swelling and to the formation of new blood vessels growing off the retinal surface. These new blood vessels are very fragile and tend to leak fluid and break easily causing large areas of retinal hemorrhage, pre-retinal hemorrhage or vitreous hemorrhages. This in turn makes the retina more susceptible to tears and or detachments that have a low probability of be repaired successfully. Proper weight control, exercise, diet and appropriate medication can make a big difference in controlling the effects of diabetes mellitus. A person diagnosed with diabetes and no signs of diabetic retinopathy is typically seen on an annual basis for examination of the retina through a dilated pupil. Should minor changes be seen, a six-month evaluation would be recommended. More frequent examinations will be recommended if the retinopathy is close to needing treatment with lasers or intra-ocular medications. Should the retinopathy develop to the point of clinically significant macular edema or proliferative retinopathy a referral to a retinal specialist for the appropriate treatment would be necessary. Copyright © 2013-2023 by Brian Van Dusen, O.D. and CitiVU. Hot-links are welcome. All rights reserved. Some images © Skypixel & Rob3000 | Dreamstime.com Last Change: 27 November, 2013 | |||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||